Table of Contents
How to Detect Cervical Cancer in Older Adults.
What is the Cervix?
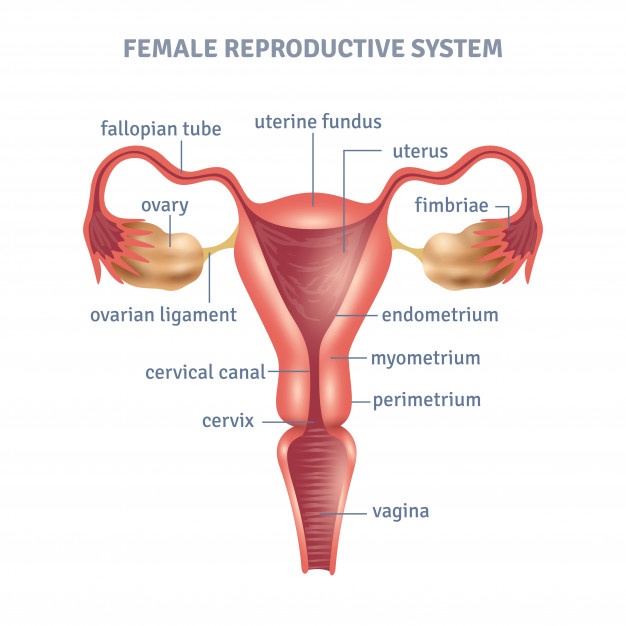
The cervix is the lowest region of the uterus, it has diverse functions in the female anatomy such as: attaching the uterus to the vagina, keeping bacteria out from the uterus and it also helps in cleaning the vagina.
What is Cervical Cancer?
Cervical cancer is an abnormal growth of cells in the cervix, this abnormal growth can be caused by many factors which leads to cervical cancer.
Summary
- Statistics lead us to believe that cervical cancer is a relatively common cancer in females who are 50 years and above.
- Cervical cancer is caused by late diagnosis and treatment of a cervix infected with human papillomavirus. Human Papilloma Virus also known as HPV is a virus that is mainly transmitted by sexual intercourse.
- Cervical cancer is treatable if detected and diagnosed early before it spreads to other parts of the body.
SEE ALSO: How to Detect Prostate Cancer In Older Adults
Factors contributing or leads to cervical cancer
Some of the factors that contributes to the growth of cells in the cervix that in turn leads to cervical cancer are:
- human papillomavirus (HPV): human papillomavirus (HPV) is a sexually transmitted infection that is contracted from an infected person during sexual intercourse, this infection is treatable if diagnosed on time but it can not be cured.
- Smoking: Research shows that women who smoke has some deposit of tobacco in their cervical mucus and this affects the cells in the cervix. The changes in the cells of the cervix could lead to cervical cancer.
- Early marriage: A girl child that is married out early is at a high risk of contracting sexually transmitted infections (STI) such as human papillomavirus (HPV) and has a higher chance of multiple childbirths. As these are both risk factors for cervical cancer, we can infer that early marriage increases the risk.
- Multiple child birth: Pregnancy is thought to be a period of lower immunity and a lot of hormonal change. This is believed to predispose a woman to cervical cancer. It may also be believed that the number of times a woman’s cervix has to pass through changes from childbirth could increase the risk for cervical cancer.
- Early sexual relationships: A woman that had engaged in early sexual relationships is at risk of contracting Human papillomavirus (HPV) without any signs and symptoms until much later.
- Socio-economic status: With finance, it is possible to carryout regular examination of the cervix and commence early treatment for any anomaly. However, with low income, people are unwilling to commit funds or time to do regular checks.
- Long term use of birth control pills: Most birth control pills are synthetic hormones which might encourage the growth of cancers.
Stages of cervical cancer with treatments.
As with most cancers, there are 4 main stages. Stage one being at the beginning and stage four being the end stage of cancer. In this article we include a stage zero which is called the pre-cancer stage.
Stage 0: In this stage, the human papillomavirus is still growing in the cervix, it is referred to as pre cancer stage.
Treatment
At this early stage, Cryotherapy, Conization, Laser therapy and Loop Electrosurgical Excision Procedure (LEEP) may be used.
Stage 1: At this stage, the cancer is found in the cervix and the size of the tumor increases to about 5millimeters deep.
Treatment
Surgical procedures to get rid of the cancer cells.
Chemotherapy: The use of drugs to destroy cancer cells.
Radiation: The use of radiation to kill or shrink cancer cells.
chemotherapy is used alongside radiation for effectiveness.
Stage 2: At this stage, the cancer cells have spread to the upper part of the uterus known as the corpus or fundus to about 4 centimeters in length.
Treatment
Chemotherapy and radiotherapy can be administered but if the growth of the cancer cells keep increasing then hysterectomy, radical trachelectomy, Exenterating, Bilateral salpingo oophorectomy may be required. These are medical procedures for the removal of the affected areas.
Stage 3: At this stage, the cancer cells have affected most of the areas surrounding the vagina, it also blocks the ureter (the organ that helps the passage of urine from the kidneys to the bladder. At this stage also, since the ureters are affected, if proper management and care is not taken it can affect the kidneys and stop the kidneys from carrying out its functions.
Treatment
Even though in this stage, the cancer may have gotten more aggressive, a combination of chemotherapy and radiotherapy is used.
Stage 4: This is the final (metastatic) stage of cancer growth. At this stage, the cancer cells have spread to other parts such as the bones, bladder, lungs and lymph nodes.
Treatment
At this stage, a combination of all the other methods may be used alongside medication to reduce pain.
Symptoms of cervical cancer in older-adults
You probably won’t see indications of cervical cancer until it’s far along. They might include:
- Pains when you engage in sexual intercourse
- Surprising vaginal bleeding, for example, after sex, between periods, after menopause, or after a pelvic test
- Surprising vaginal discharge
After the cancer has spread, the following may be experienced:
- Pelvic pain
- Inconvenience peeing
- Enlarged legs
- Kidney failure
- Pain in the bone
- Weight reduction and absence of hunger
- Exhaustion
Ways to prevent cervical cancer
Cervical cancer is caused mainly by the growth of cancerous cells in the cervix known as human papillomavirus (HPV) and this is mainly gotten from sexual intercourse, below are some of the preventive measures:
- Pap smear: Pap smear test should be carried out regularly by women from their late forties, this will help to diagnose and administer treatment timely before the cancer worsens.
- Avoid numerous sexual partners: Human papillomavirus is transmitted through sexual intercourse, having numerous sexual partners increases the risk.
- Quit smoking: Smoking tobacco have been shown to reduce the activity of the immune system, quitting smoking tobacco will help the immune system to fight against the growth of the human papillomavirus (HPV).
- Abstinence from early marriage and early sex: Being sexually active very early is a risk factor for contracting the human papillomavirus virus (HPV), and potentially developing cervical cancer later on. Abstinence will help reduce this risk.
Frequently asked questions (FAQs) on cervical cancer in older-adults
Why are cervical cancers difficult to detect in Older Adults?
Most people report late to hospital with cervical cancer because the symptoms are not aggressive initially and can be mistaken for other things (e.g.) menopausal symptoms. However, medically it is possible to detect cervical cancer as well as treat it.
Can I detect cervical cancer without any tests?
Tests are needed to confirm the cervical cancer diagnosis. That notwithstanding, some symptoms like pelvic pain, strong smelling and blood-stained vaginal discharge, bleeding at irregular times such as after sex, between periods; may be an indication for further investigation to be done.
How often do I need a pap smear?
People younger than 20 years old rarely develop cervical cancer. The risk of contracting HPV goes up when people become sexually active, this is usually between the teen age and mid-30s.
Women who are 21 years and above are required to carry out cervical cancer screenings, which include a Pap test and/or an HPV test. Once in every 3-5 years if the last test showed no HPV and after women get to 65 years, they may not be required to take further tests if their test results show no HPV.
Is there a vaccine against cervical cancer?
There is a vaccine for HPV which is the culprit for cervical cancer. According to BBC news, this vaccine is cutting cases of cervical cancer by 90%.
Final thoughts
Pelvic test and pap smear should be done periodically by women above the age of 50.
Even if you are below 50 years old and you have any of the symptoms of cervical cancer, we advise you consult your doctor who will based on your symptoms and his/her experience recommend further tests and treatment plan.
Self-medication and local-remedying are one of the causes of late diagnosis and treatment and accounts for a lot of deaths.
Suggested further reading: visit cancer.net

